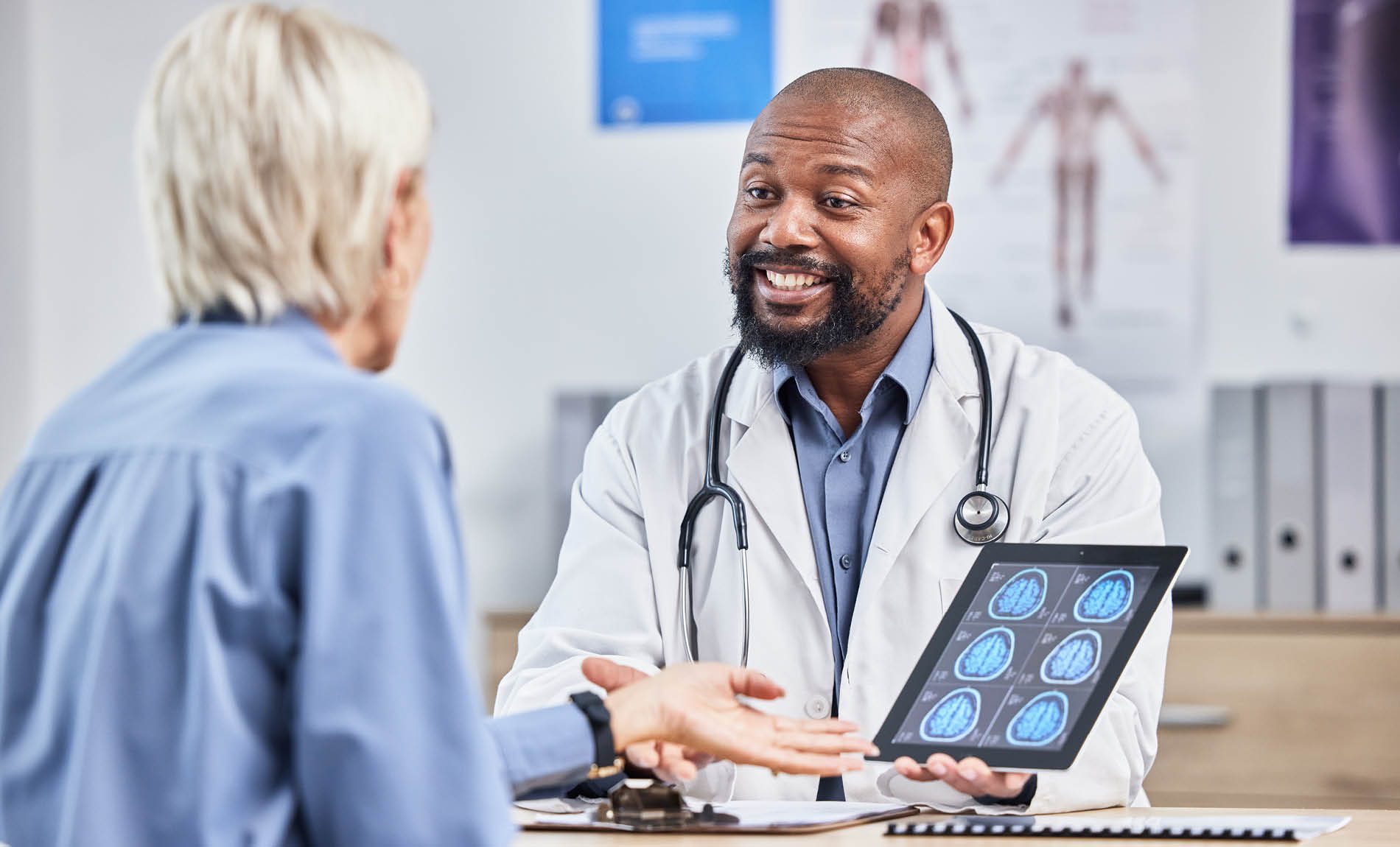
In our September edition of FORTIS magazine, Community Diagnostic Centre insiders Michael Wood, Jonathan Gardner and Nicola Theron reflect on their experiences of delivering NHS services differently.
WORDS: LAUREL IVES
Community Diagnostic Centres
Community Diagnostic Centres (CDCs) are a growing success story – even with the many challenges facing the NHS in its 75th year. The concept for CDCs was first mooted by the NHS’s then-cancer tsar, Professor Sir Mike Richards, in his review of NHS diagnostics capacity in October 2020. And in that time we’ve witnessed shifting attitudes to healthcare and how it is delivered.
“Looking back, the pandemic was a key moment when people’s minds were changed,” says Michael Wood, Head of Health Economic Partnerships at the NHS Confederation. “I had my first vaccine jab at the racecourse and the second one in a shopping centre; citizens realised they don’t need to go to a typical clinical site to receive healthcare, and people really grabbed hold of that. NHS managers began to ask: what other services can we move to the high street?
“Can we offer quicker testing? Can we change a unit to offer scanning and blood testing without some of the restrictions you need for traditional healthcare settings? Covid-19 showed local leaders they can experiment with different ways of trying to deal with the pressures they are facing,” he says.
Health leaders also recognised that the CDCs were a useful way to reach underserved communities who may struggle to travel to a hospital or be put off by a more formal healthcare setting. Says Michael: “It’s not just about what services the NHS needs to provide, but where we should provide them. Different populations have different needs. There are communities we struggle to reach. We may not know about them and inequalities may be widening – this is a key part of narrowing those inequalities.”
The CDCs now
CDCs have been opening at pace since 2021. In June this year the government announced that 108 CDCs are in operation and have already delivered more than four million additional checks for a range of conditions, from cancer to heart or lung disease.
More than 40 new CDCs are due to open. Some of the centres are in football or rugby grounds, some are in leisure centres, some are in shopping centres and some are attached to hospitals, but with separate entrances and exits so they can operate independently.
“It’s about partnering with councils and local communities to understand the best location for the CDC,” continues Michael. “I visited the one in Wood Green shopping centre in North London recently. It was in an old Phones 4U shop and it opened last autumn, performing blood tests, eye tests and x-rays.
“CITIZENS REALISED THEY DON’T NEED TO GO TO A TYPICAL CLINICAL SITE TO RECEIVE HEALTHCARE”
Now they’re developing the room downstairs for an MRI scanner. I walked past recently and just did a double-take – it was bustling and just felt so un-NHS-like, and that is something to celebrate I think.”
Shopping for health
Situating the Community Diagnostic Centre in a shopping centre like the Wood Green CDC is not only convenient for local people, but also an advantage for the centre itself. “The CDCs open up new approaches to widening access. Patients can be referred by their GP to a centre in their own community, which also acts as an advantage for their local high streets as initial research in some settings found more than 50% of patients stayed in the shopping centre after their appointments and did some shopping or had a bite to eat.
“It provides extra capacity for the health service, reduces waiting time and provides significant footfall through the high street or shopping centre. It’s a win-win,” says Michael.
Engaging with the local community is also an important factor in deciding where the centre should be and what services they might need.
“For example, if a community has a high propensity for diabetes, we might need slightly different services there, and that is all part of the journey,” says Michael.
Three models for CDCs
That said, the CDCs must conform to one of three archetype models. A standard model offers a minimum of tests and scans, including CT, MRI, x-ray, blood tests, respiratory and cardiology. A large CDC can also offer endoscopy and any other diagnostic testing that is required in the local community, as well as scalability, such as multiple scanners to improve efficiency.
The final archetype is for a ‘hub and spoke’ model, where the ‘hub’ includes all minimum testing and then a series of ‘spokes’ provide further capacity for tests with satellite locations, mobile units or pop-ups. These can be useful for large geographical areas.
Despite the drive to situate CDCs in the local communities, in some areas the best place can still be the local hospital.
The Finchley Memorial Hospital CDC opened in north London in August 2021 and now offers patients two MRI scanners along with two obstetric ultrasound machines.
In addition to this, the hospital is serving the local community with a direct bus route to the CDC, as well as pre-bookable, free parking on site. And crucially the CDC must have a separate entrance and exit to the hospital so that it’s not impacting the acute site. In August 2022, just one year after its arrival, the Trust announced that they had reached 50,000 patients, making a real impact on the local community.
Jonathan Gardner, who leads on delivery of CDCs in north London, told the Times Series: “Every one of these appointments has supported our hospitals to recover from the impact of the pandemic and improved access to diagnostic tests for our patients.”
Michael believes the CDC has a vital part to play in the current workforce shortages facing the NHS. “Being in town centres allows us to be more visible and that can help us recruit. We can say to people: ‘Hey, we have 350 different careers in the NHS, come and join us’.”
He hopes that the opening of the CDCs will prompt some long-term strategic thinking about local communities and NHS estates.
“Lots of hospitals and NHS buildings are very old, with a backlog of repairs worth more than £10 billion. This along with the workforce struggle are two of our biggest challenges. Unlocking new NHS estate and going into local communities gives us a potent business case for future long-term change.”
“IT WAS BUSTLING AND JUST FELT SO UN-NHS LIKE.”
© Dialogue Content Marketing Ltd 2023.
This article was taken from the September 2023 edition of FORTIS magazine.
FORTIS magazine is a Health Spaces Limited publication. Opinions expressed in FORTIS magazine are not necessarily those of Health Spaces Limited or Dialogue Content Marketing Ltd. Material contained in this publication may not be reproduced, in whole or in part, without prior permission of the publishers. No responsibility can be taken on behalf of advertisements printed in the magazine.
FORTIS magazine – read more
This Health on the High Street column was written for the autumn 2023 edition of FORTIS magazine; a forum for the NHS to share ideas, innovations and case studies. To read the publication in full and access a digital copy, visit FORTIS magazine. FORTIS magazine is free for NHS change-makers and leaders and is available as a print or digital copy. FORTIS magazine is managed and owned by Health Spaces Ltd.
Please note: Health Spaces is pleased to showcase projects we have worked on and also to be able to share projects and developments which we have not been involved with. The NHS Health on the High Street schemes named in this article are not Health Spaces projects.