As hospitals face rising demand and increasingly complex patient needs, a critical design question is often overlooked: how well does the built environment support the safe, dignified movement of patients? This article explores why patient handling must be embedded at the earliest stages of estate planning and how doing so strengthens safety, efficiency and the everyday experience of care.

Healthcare estates are under increasing pressure to accommodate rising demand, growing patient complexity and sustained operational strain. Much of the current conversation centres on digital transformation, automation and clinical innovation. Yet beneath these high‑profile themes lies a question that is fundamental, and often far less explored: how effectively does the built environment support the safe, dignified movement of patients, and what are the consequences when it doesn’t?
Drawing on Innova’s experience supporting major hospital projects, this article reflects a frontline understanding of how estate design shapes everyday patient movement. Patient handling is one of the most routine, high‑frequency activities in healthcare. It shapes staff wellbeing, patient experience, operational flow and clinical risk. And yet, across many estate programmes, it remains a secondary consideration; addressed late in the design process, or worse, only after teams encounter avoidable friction once a building is already in use.
When patient handling is not embedded from the start, estates may meet its technical specifications but fail to support the realities of everyday care, creating inefficiencies that are difficult and costly to resolve post-build. What is required is not simply better equipment or isolated interventions, but a shift in mindset: patient handling must be treated as a core design principle that informs the earliest decisions in estate planning, not a logistical detail applied after the fact.
The hidden architecture of patient movement
The movement of patients – whether assisted, supported or fully dependent – is deeply shaped by the physical logic of a healthcare building. Corridors, turning circles, bed and trolley routes, lift positioning, room proportions, door widths and structural loadings all influence how safely and efficiently patients can be moved. These decisions are often invisible once the building is complete, yet their impact is felt constantly by staff.
Modern healthcare demands have made this more important than ever. Higher acuity cases, shorter lengths of stay, more rapid transitions between departments and an ageing, less mobile population mean staff undertake more transfers and manoeuvres. When the built environment is not aligned with these needs, inefficiencies accumulate quickly:
- Transfers take longer.
- Double‑handed work becomes unavoidable.
- Staff fatigue accelerates.
- Patient dignity diminishes.
- Operational bottlenecks emerge without any technology or process able to compensate.
A space that looks functional on a drawing can behave very differently in practice. What appears workable in a design review can become restrictive or unsafe during an actual transfer involving real equipment, real patients and real-time pressures. For frontline teams, poorly considered layouts are not inconveniences; they are everyday friction points that shape how care feels and how safely it can be delivered.
Operational consequences of late-stage decision-making
In many estate programmes, the integration of handling systems happens after core architectural features have already been decided. At that point, the easiest path becomes adding mobile equipment rather than rethinking the underlying spatial logic. While mobile hoists and transfer devices have a role, they cannot compensate for a building that has not been designed around patient movement from the outset. They occupy floor space, require storage, depend on staff availability, and often increase the physical load on caregivers instead of reducing it.
By contrast, ceiling track hoists, when integrated early, provide continuous support without intruding on the space. They allow movement to become embedded into the architecture rather than added to it. But their success depends entirely on early decisions: the position of structural beams, the strength of ceilings, the width of rooms, the direction of travel between bed spaces and bathrooms, and the ability to future‑proof routes as patient needs evolve.
Retrofitting such systems is often prohibitively disruptive or structurally impossible. Even when feasible, it rarely achieves the same coverage, functionality or cost‑efficiency as early design integration. The question, then, is not whether patient handling equipment is valuable; but whether estates teams are given the opportunity to design the building around the movement needs it must support.
Designing for complexity, bariatric care and future demand
Patient complexity is rising across the NHS. Bariatric care, in particular, is expanding year on year, placing significant demands on estates that were not designed to accommodate larger equipment, greater movement space or higher‑load systems. Standard room proportions that were once considered adequate can become limiting or unsafe.
In this context, designing for handling is not a matter of preference; it is an essential component of resilience. Rooms must support staff of differing physical strength, working with patients of differing mobility, using equipment that must be manoeuvred smoothly, safely and without compromise. The estate must absorb variation without creating risk. Future‑ready estates treat patient movement not as a niche consideration but as an organising principle: one that shapes space, informs circulation patterns and anticipates clinical scenarios that may change across the lifespan of the building. When estates teams embed these requirements early, the resulting environment is not simply compliant but adaptable, capable and dignified.
Designing with movement in mind
A recent example can be seen at Midland Metropolitan University Hospital, where Innova Care Concepts worked in partnership with project stakeholders to ensure patient handling was embedded into the design from an early stage. By partnering with Innova during the design phase, the project team ensured that ceiling track hoists were integrated into key clinical areas as a strategic component of the building rather than an addition.
This approach did not simply ensure that equipment was present; it re‑shaped how space was conceived from the beginning. Structural requirements were aligned early, ensuring the hoists could be supported without compromise. Circulation routes were planned with movement as a central design driver, allowing staff to transfer patients between bed spaces, bathrooms and clinical zones without interruption or awkward detours. Coverage was mapped holistically, creating a network of movement that felt intuitive for staff and seamless for patients. For clinicians, this meant safer working practices and greater independence, reducing the need for double‑handed transfers and lowering the physical strain inherent in manual handling. For patients, the experience became more predictable, more controlled and more dignified – a smoother transition that respected their comfort and autonomy. These improvements were not the by‑product of equipment alone, but of when and how movement was integrated into the estate.
The lesson from Midland Metropolitan is clear: coherence is only possible when estates leads, clinicians, designers and patient‑handling specialists collaborate early enough for movement to influence the fundamental shape of the building. Once layouts are fixed and construction progresses, opportunities for such alignment narrow rapidly. Early design decisions determine whether patient handling becomes an enabler of care, or an enduring source of friction.
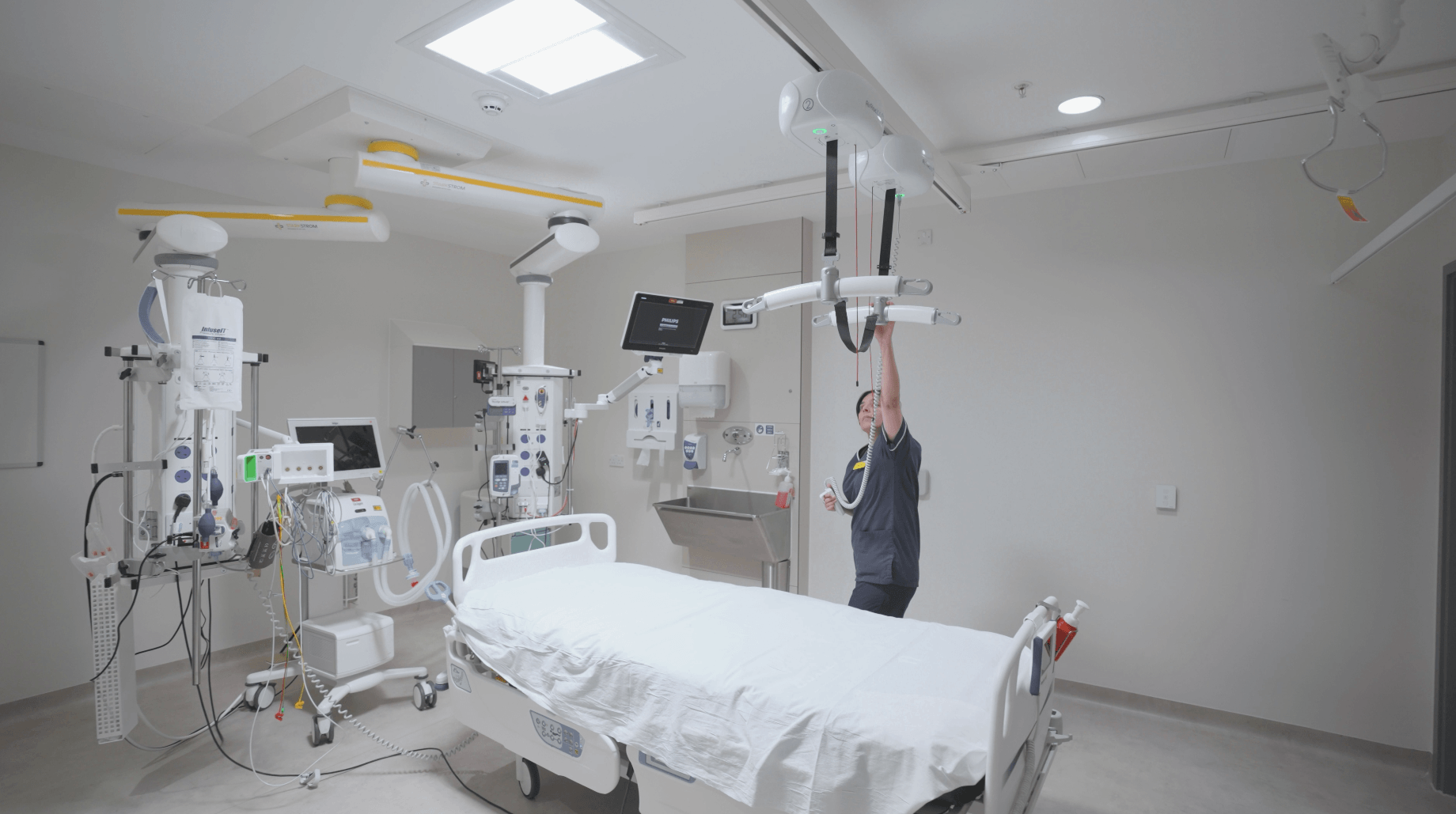
Toward a more integrated approach to healthcare design
For the NHS, the implication is clear. Patient handling cannot continue to sit at the margins of estate planning if healthcare environments are to meet the demands placed upon them. It must be recognised as a core component of how healthcare environments function and designed accordingly from the outset. This requires a shift in how projects are approached. Handling considerations need to be brought into the earliest stages of design, when spatial layouts, structural requirements and clinical adjacencies are still being defined. At this point, movement can shape the building in a way that supports safe, efficient care. Once these decisions are fixed, the opportunity to do so is significantly reduced.
It also requires stronger collaboration between estates teams, clinicians and specialist providers. Patient movement is not a single discipline issue. It sits at the intersection of design, operations and workforce realities. Treating it as such enables more coherent environments, where workflow and care delivery are aligned. Crucially, patient handling should be understood as infrastructure rather than equipment. It is not an addition to the estate, but a defining element of how it performs. When this perspective is adopted, the focus shifts from meeting minimum requirements to creating environments that actively support staff and patients in everyday practice. Healthcare estates are not passive settings; they shape how care is delivered in real time. Designing with patient movement in mind ensures that environments are not only compliant, but capable of consistently supporting safe, efficient and dignified care at scale.